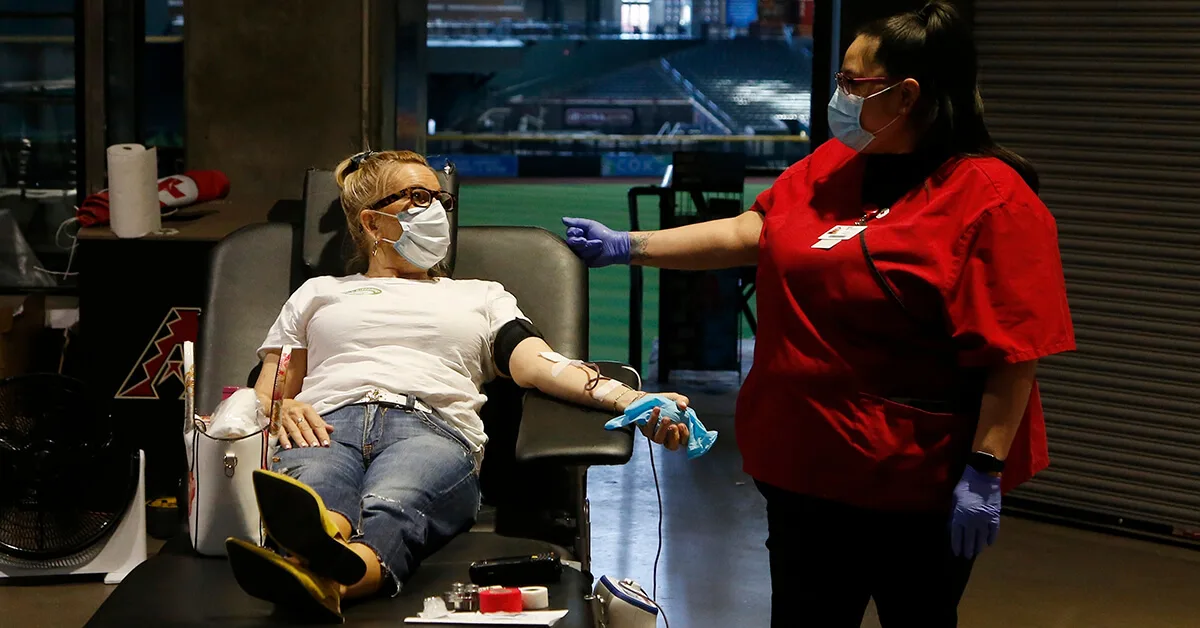
AP Photo/Ross D. Franklin
Some studies show that plasma therapy may speed recovery time for COVID patients, which is why Arizona blood-donation organizations are collecting blood that hospitals can administer.
As vaccinations for COVID-19 continue nationwide, blood donation agencies are stepping up efforts to encourage those who’ve had the disease and recovered to donate their plasma to help treat the sick.
January is National Blood Donor Month, a time when agencies typically work to recruit more donors as bad winter weather and seasonal illnesses reduce donations. This year, the American Red Cross and other groups are heightening calls for donations of blood and plasma, the liquid portion of blood, which contains antibodies that can fight off infections.
The Food and Drug Administration has authorized convalescent plasma therapy for COVID-19 on an emergency basis. Some studies show that plasma therapy may speed recovery time for COVID patients, but research is ongoing, and one study published in November in the New England Journal of Medicine found no significant differences between those who received plasma and those who did not.
Vitalant of Scottsdale and other blood-donation organizations are collecting blood that hospitals can administer.
“It’s an emergency need for more convalescent plasma donors, especially now as we’re seeing cases rising,” Vitalant spokeswoman Sue Thew said. “As people recover, that’s one way that they can give back in a way that nobody else can.”
Phoenix police Officer Santos Robles contracted COVID-19 in July and experienced life-threatening symptoms that twice put him in intensive care. He said he received five plasma transfusions and believes with each procedure, his health improved.
“It shortens the symptoms that you have,” Robles said. “The fevers start to kind of dissipate, and you start feeling a little bit better.”
Carlos Sanchez, director of public affairs in Hidalgo County, Texas, received a plasma transfusion after contracting COVID-19 this summer. He remembers feeling better but isn’t sure whether the benefits were real or psychological.
“I don’t know that (the symptoms) disappeared magically, but in my mind (they) did,” Sanchez said. “I just felt a cool feeling. … Whether it had ancillary, physical help, I’ll never know.”
Clinical trials, including one overseen by researchers at Vanderbilt University Medical Center, are continuing to determine whether plasma transfusions have real benefits.
Dr. Marilyn Glassberg Csete, chief of pulmonary medicine at the University of Arizona’s College of Medicine, said more proof is still needed.
“They can’t say there is evidence unless there’s a randomized, double-blind, robustly constructed and conducted trial,” she said.
The donation itself takes about an hour, and donors must have been symptom-free for at least four weeks.
Robles recently donated blood in hope of paying it forward.
“Somebody wanted to help somebody when they donated the plasma that I got,” he said. “So therefore, if the plasma that I give helps somebody, that’s the goal – because it helped me.”

He said what? 10 things to know about RFK Jr.
The Kennedy family has long been considered “Democratic royalty.” But Robert F. Kennedy, Jr.—son of Robert F. Kennedy, who was assassinated while...

Here’s everything you need to know about this month’s Mercury retrograde
Does everything in your life feel a little more chaotic than usual? Or do you feel like misunderstandings are cropping up more frequently than they...

Arizona expects to be back at the center of election attacks. Its officials are going on offense
Republican Richer and Democrat Fontes are taking more aggressive steps than ever to rebuild trust with voters, knock down disinformation, and...

George Santos’ former treasurer running attack ads in Arizona with Dem-sounding PAC name
An unregistered, Republican-run political action committee from Texas with a deceptively Democratic name and ties to disgraced US Rep. George Santos...




